From left to right: Allison McGeer, Benita Hosseini and Christina Guzzo
May 11, 2023
By Betty Zou
On Friday, May 5, the World Health Organization declared the end of the COVID-19 global health emergency.
We polled faculty members of the Emerging and Pandemic Infections Consortium (EPIC) and the Institute for Pandemics (IfP), two pandemic-focused Institutional Strategic Initiatives at the University of Toronto, to get their perspectives on the WHO’s decision and where we need to go from here.
The 28 experts who responded to our poll are clinicians, clinician scientists, engineers and scientists who work in areas such as epidemiology, infectious disease biology, immunology, and public and community health. Their answers capture a moment in time when the pandemic has receded from the center of public discourse, but the virus is still causing excess hospitalizations and deaths and many are still dealing with the long-term consequences.

When asked whether they agree with the WHO’s decision to end the COVID-19 global health emergency, half of our experts agreed or strongly agreed. Roughly one-third expressed disagreement with the WHO declaration and 14 per cent were neutral.
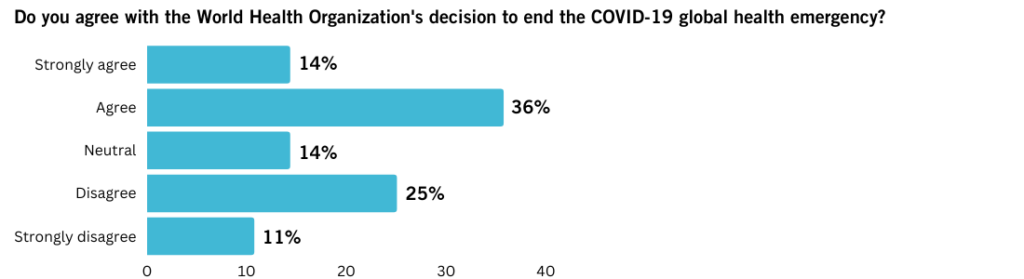
We also asked our experts what COVID-19 precautions they are still practicing today. Nearly all respondents said they are staying up-to-date with boosters as recommended and staying home when they’re sick. Three out of four said they use rapid antigen tests when necessary. Unsurprisingly, the question of masking had the least consensus with one in two experts continuing to mask indoors.

Looking forward, we asked our experts how prepared they felt Canada is to deal with future emerging infectious threats and/or pandemics. Although close to 40 per cent of our experts felt Canada was more prepared to handle another outbreak than before COVID-19, an equal number saw no improvement in our ability to respond and almost 20 per cent of respondents believed that the country is less prepared now than it was three years ago to deal with future pandemics.
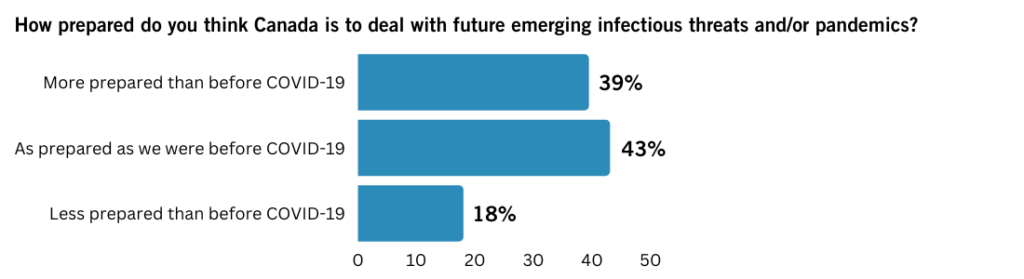
Our poll also included two questions about key learnings we should take away from the COVID-19 pandemic and what we should do now to ensure that we are more prepared next time.
Equity was a common theme that emerged from the learnings that were shared. “The very clear and large inequities in illness and death by income and race in Canadians were dramatically obvious during COVID-19, but they exist for all diseases,” said Allison McGeer, an EPIC member and professor of laboratory medicine and pathobiology in the Temerty Faculty of Medicine at U of T.
Benita Hosseini, an IfP member and an assistant professor in the department of family and community medicine, shared one of her main takeaways about surveillance. “The COVID-19 pandemic has taught us a crucial lesson: we urgently require a well-functioning early threat warning system. It’s been three years since the pandemic started, yet we still lack a functional nationwide system.”
Other lessons from the pandemic focused the importance of responding quickly and delivering clear and consistent messaging to the public. Several experts also reflected on how the pandemic highlighted gaps in the public’s understanding of science and public health and the need for more education in these areas to build trust and combat misinformation.
When it came to the question of what we can do now to strengthen preparedness, the responses were clear – invest in our healthcare system and invest in research.
“We need to prioritize investment and focus on strengthening public health infrastructure,” said Hosseini, who is also a scientist in the Upstream Lab at Unity Health Toronto. “This includes increasing funding for healthcare systems, implementing multiplex rapid antigen testing in primary care and emergency departments, increasing the capacity of laboratories and research institutions, and improving healthcare access and equity.”
Christina Guzzo, an EPIC member and assistant professor in the department of biological sciences at U of T Scarborough, shared a similar sentiment. “Invest in science and technology, establish the collaborations and pipelines for more rapid and streamlined responses, and support trainees and emerging researchers to build careers in these fields so they can help respond in future.”
Together EPIC and IfP are working to address the gaps identified by our experts to prevent and prepare for future pandemics. Through funding, training and collaboration opportunities, we are advancing innovative, interdisciplinary research on emerging and existing infectious disease challenges, from surveillance and diagnostics to pathogen biology and host immune response to post-pandemic recovery and societal impacts of outbreaks. U of T is also home to the newly established Canadian Hub for Health Intelligence and Innovation in Infectious Diseases (HI3) that brings together over 80 partners to strengthen pandemic preparedness and increase Canada’s biomanufacturing capacity.


